Had an interesting case today.
A 28 year old guy with a condition called fascioscapulohumeral dystrophy.
He was having a unilateral thoracoscapular fixation, and having never done this before, I wasn’t sure which block(s) to do, or even if it was possible to cover this surgery with a regional technique.
The incision is a paramidline incision, between the vertebral border of the scapula and the midline of the spine, extending from C7 to T6.
To demonstrate, this image was taken from a case report (Brachial Plexopathy Following Thoracoscapular Fusion in Fascioscapulohumeral Muscular Dystrophy, G.I Wolf et al, Neurology, Feb 2005)
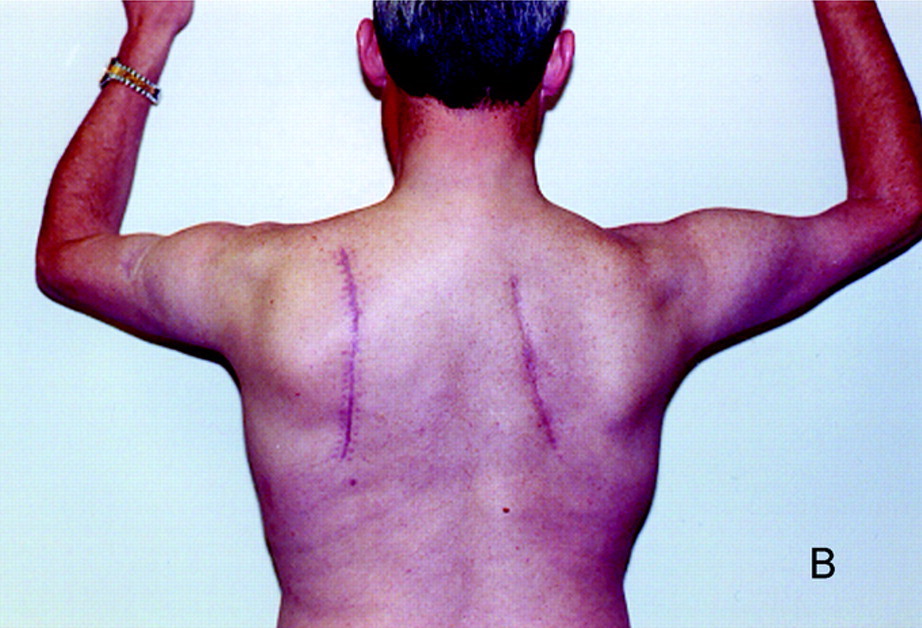
So, I guess the question is, would you offer a block to this patient? If yes, which block or combination of blocks would you go for?
It would be great to hear some expert opinions!
Ill post again later with the details of what I ended up doing, which I’m glad to say was very successful !
Billy Qureshi
8 thoughts on “FascioScapuloHumeral Dystrophy”
Follow the discussion here too…
https://mobile.twitter.com/NUSGRARVI/status/900122186635243520
I don’t think any single block would cover it fully. Given the superficial and deep nature of surgery in a mobile region, with multiple muscles (splits) of different innervations, then fixation with restriction of movement.
Hopefully if it were a more lateral incision (e.g. the one on the left in picture above) – then regional techniques could be opioid sparing. I’d try unilateral paravertebral block (T2-T4), and suprascapular nerve block. I’d need some help with the latter, as I’ve never done one (successfully).
Is this a good indication for ESP block I wonder. Not done any either – but uncertain if advantageous in this case
Hi Lewis. So yes you’ve basically mentioned the block combination that I used. Which was a superficial cercical plexus and an ESP (not a PVB only because I had poor Ultrasound equipment!!). But – it worked perfectly. Was quite surprised. Thinking ESP could be utilised in rib fracture patients and almost certainly will be easier to leave a catheter in this location! What do you think?
I agree, I have done both PVB and Erector spinae for incisions in this region. I am not entirely sure of the place of ESPB but one thing I am certain of is that it numbs the posterior branches of the spinal nerves. Supraclavicular nerve would probably needed. The boney pain is a bit more tricky as it may have some contribution from brachial plexus bracnches. However in my limited experience a combination of supraclavicular and paravertebral works for scapular fractures
As above, for the skin you would need to cover the posterior branches of the spinal nerves (PVB / ESP). I’m not sure whether you strictly needed the supraclavicular nerve from cervical plexus (and potential phrenic etc. risks) – it depends which anatomy diagram you look at. You might do for the higher one on the left, but the one on the right seems too low to me.
Bony innervation would be a combination of spinal nerves and brachial plexus (suprascapular n block) – I’d ask the surgeon exactly what they were attaching to what. Obviously you didn’t need it for your patient.
morphine?